Explanation
Program billing is used to automatically create a claim with a predefined rate for EVERY day a client is enrolled in the program. This set up is completed after the following windows have been completed per standard workflow. Once the program billing configuration is complete notify Remarkable Health to activate the process.
- Program Clinical > Program
- Service Type Billing > Maintenance > Service Type
- Procedure Code Billing > Maintenance > Procedure Code
- Billing Matrix Billing > Maintenance > Billing Matrix
Configuration
Access: Billing > Maintenance > Program Billing
1. Click the Add button.
2. Enter the following information:
Description
Enter a description to identify the record.
Program
Select the Program from the drop down list.
Effective Date
Enter the date the billing will begin for this program.
Expiration Date
This field can be left blank until the program is expired or the billing is processed in another manner.
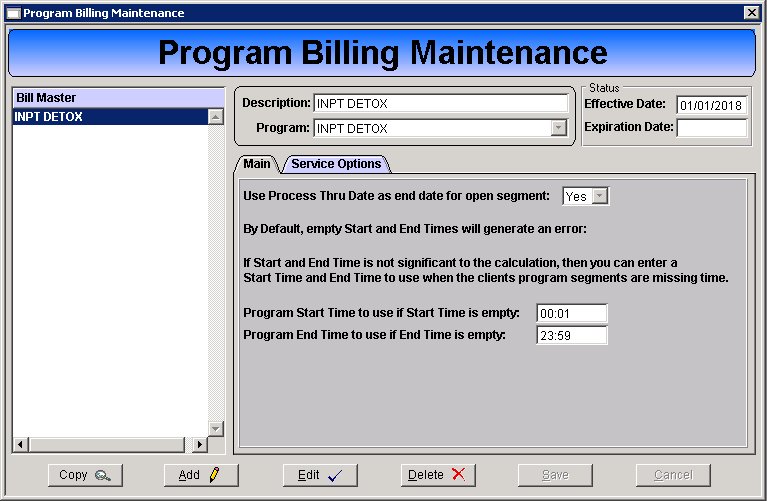
3. Complete the Main tab.
Use Process Thru Date as end date for open segment
Select "Yes" unless otherwise instructed by Remarkable Health Support.
Program Start Time to use if Start Time is empty
Enter 00:01 for a full day/per diem rate.
Program End Time to use if End Time is empty
Enter 23:59 for a full day/per diem rate.
4. Click Save.
5. Open the Service Options tab.
6. Click the Add Service button. The Program Billing Detail Maintenance window presents.
a. Select the Service Type from the drop down list.
b. Select the Day Span Type.
- Bill as Day Span - This option creates a single claim line with the date span and calculated units.
-
Bill Individual Days - This option creates individual claim lines for each day of the date span with a single per diem unit.
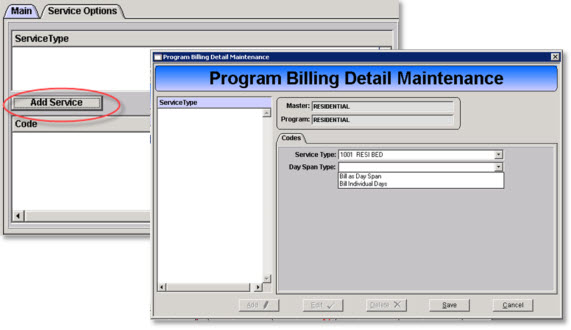
c. Click Save.
7. The Detail Maintenance window closes.
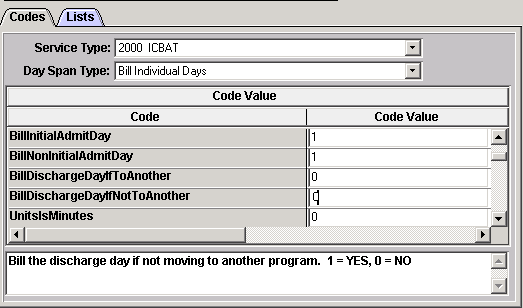
8. The Code Value table opens.
9. Click the Edit button.
10. Click in the Code Value field for each code line to view the description of the value. Enter the appropriate value based on the value description and options.